11/3/2009
Dear Shari and Toby,
BACK PAIN
When I was twenty six I was retrieving Little Bit, my Siamese cat, from the second story of the apartment building. It had been raining and the bare wooden steps were slick. I held the cat next to my chest with both arms as my foot slipped off the top step. I tried to keep my balance by raising my right leg out in front of me but the pants I had on bagged a little causing my left leg to be pulled from under me when they tightened. I landed on the edge of the second or third step. All I could see were bright flashes of light as I bumped down the rest of the steps to the bottom. I could not get up without help from your mother who helped me into the first floor apartment. I was in a lot of pain for a couple of months but was able to make it to work most days. My neck and back would get so sore I could hardly stand it. After a few months I found I could make it through the day if I braced myself on the arms of the chair. By then I had seen several doctors who could find nothing wrong with my back. X-rays were not very clear then. The next three or four years were tough and filled with pain. After about seven years most of the pain was gone.
When I was forty two, your mother gave me a membership to a racket ball club. She knew I loved to play. I spent most of my time behind a desk and my lower back was not in good condition. I managed to strain my back and created a herniated disc. The doctor wanted to operate on it. Looking back, I am glad I did not take his advice. I have known many others who did. All of them are in as much pain and discomfort as I am now (which is only annoying, not severe) and are more restricted in their movement due to the increased strain and risk of damaging the next vertebra above the fused one. Some were not told of this consequence until after the operation. Out of desperation I went to see a chiropractor. This turned out to be a good idea. When he had taken the x-rays and examined them, his first question was “when did you break your back?” He showed me the crisp picture of T10 with a top portion looking like a king’s crown. Approximately one fourth of the vertebra was gone. I said it only hurt every once in a while and he then went on to treat L3. It took another seven years to learn how to care for my back.
The last thirty five years of trial and error have led to some conclusions I can safely rely on:
1. If you have a desk job you will have back problems if you do not make the effort to properly exercise it.
2. It is less painful to exercise than to cope with a bad back.
3. Exercise for a bad back should not include straining but emphasize fluid movement to provide a gentle “stirring” of the body’s chemical reactions.
4. If you have a back problem, surgery is not an option if you can walk.
5. Most of the pain from a bad back is due to inflammation and swelling. It is important to maintain a diet providing nutrients similar to fighting a disease.
6. Another large portion of the pain is due to muscle/tendon strain. This can occur from poor posture or over exertion. If you work at a desk it is important to have the desk/chair “tuned” to your needs providing an ergonomically sound chair and desk system. Carpal Tunnel Syndrome and shoulder related problems can also result from not paying attention to these needs.
7. The remaining pain is caused by pinched nerves. This can be disabling if not corrected.
8. An injured back (baring falling on steps, etc…) starts long before the pain occurs. If your back is maintained (proper exercise and rest) and your spiritual and mental condition are balanced, the back normally cannot be strained or disc bulged. It can take all the stress you can apply if it is in excellent condition. The injured back starts with a poor attitude toward diet and exercise and progresses with mental stress over money, spouse, kids, or work. Worry/mental stress create tension in muscles and do not allow the muscles to relax and rest. Over a long period of time this will result in weakened muscles and tendons. This condition allows misalignment and/or tearing of body tissue.
9. Once a back is in a weakened condition, everything creates unneeded stress. Light exercise can be too much. Additional weight carried in the front/stomach area requires four to five times the weight’s effort to maintain alignment. Mental stress magnifies the deterioration due to constant tension.
If you are reading this, you probably have already been to see a medical professional. If the cause of your discomfort is not trauma and you are able to walk you have several options and requirements to meet before returning to a whole condition for your back. If you are in pain, (which you are) physical treatment by a qualified medical professional will be needed. The following guides may be useful in determining which physical treatments to choose.
1. Surgery is not an option yet.
2. If you are out of bed most of the day, muscle relaxers are not needed.
3. Pain killers (Advil, Tylenol, or prescription) should not be taken for longer than two days in a week. If the pain cannot be tolerated, bed rest may be necessary.
4. Bulging discs always result in spinal misalignment. A chiropractor should be consulted, especially after the pain subsides. The illness is not gone, only the symptoms (pain).
Simultaneously, treatment for the attitude/spiritual illness needs to begin and progress to mental correction of habits and activities. Assuming this started long before the pain, make a list of the likely contributors to the current situation. This can include physical activities but should concentrate on attitudes and mental decisions providing an environment leading to the physical condition. Without removing the spiritual, mental, and physical stresses contributing to your condition you only have the future return of the symptoms to look forward to. The following list can provide stimulation for this process. It is up to you to pinpoint the exact definition of the contributing stress. This will be necessary in the next step to eliminate the stress.
1. A complete cure has to start with locating the attitudes allowing the condition to exist. Notice the plural is used. Illness is usually the result of more than one attitude interacting to produce the end mental choices and physical results. For example, the conscious decision to not have a tone body in a healthy weight range is usually the result of several attitudes. I don’t enjoy exercising. I like eating mashed potatoes or french-fries more than green vegetables. I don’t have control over my life/job/spouse but I can do what I want with this. The attitudes are not good/bad but facts about you. Other opposing attitudes exist and the resulting mental decision is based on the priority placed on each. Unfortunately, it is usually not until later in life when many of our resources are depleted and illness occurs that we understand a change in priorities is needed. The attitudes of I like being healthy and will exercise and eat as needed to be healthy gain in priority. The largest obstacles to being healthy are recognizing the attitudes promoting illness and choosing to reprioritize our attitudes. When these filters are correctly aligned, the decisions to be healthy are easily made.
2. Mental decisions and mental stress are based on attitudes. Poor decisions and mental stresses can only be relieved by recognizing the source and changing priorities of the attitudes providing the source. By examining your poor decisions, attitudes needing reprioritizing can be identified. Mental stress is produced when attitudes of equal priority result in no clear decision and the solution is constantly revisited and/or revised. This can be competing attitudes as to working hard to provide for the family you love and not having the proper amount of time to maintain your health. In this instance, most people’s reaction is to decide by not deciding and letting the decision be made for them “naturally”. This approach almost always leads to poor health and lost income. The only way to resolve this dilemma is to struggle with the attitudes and resulting decisions until a clear balance is defined and implement that decision without constantly second-guessing yourself. Not deciding, is like the man sitting on the dock day after day watching the ship sail beyond the horizon and wondering what life would have been like if he had sailed when he had the chance in his youth. He not only lost the opportunity to sail but lost the opportunity to have a wonderful life on shore. Even a less than optimal decision is better than no decision. Make an informed decision and move on.
3. Physical stress is usually the easiest to determine. It is the trigger, shooting pain throughout the body and destroying tissue. The gun was conceived in attitudes and loaded by mental decisions. The key to pinpointing the exact stress is realizing that it is usually a day or most likely two days after the physical stress is applied before the resulting pain. You do something strenuous and you are OK. Two days later you do something much lighter and POP! The light and simple task is not what strained your back. It is simply the straw that broke it. The number one physical stress affecting the lower back is extracurricular activity with your spouse. If you want to continue without fear of later pain, the illness must be cured. The second most common physical stress is being overweight. This is a two-fold detriment by deterring exercise and multiplying stress constantly on the lower back.
In my case, I have minor constant pain in my lower and upper back (the two old injuries) and left leg pain along the sciatic nerve with numbness on the left side of my foot. Since I have all the symptoms, I strongly suspect C1 and C2 are out of alignment. The Chiropractor will have to determine if they are in need of adjustment. I have significant neck pain and headaches.
1.
Attitude – I will have to place a higher priority on regular exercise
specific to the back and neck.
2.
Mental decisions – I am no longer active enough daily to obtain
sufficient exercise. I will need to exercise for the sake of exercise itself.
- It is useless to go to a chiropractor and adjust the spine until I obtain
additional tone in the back and neck muscles.
3.
Physical – Create an area in the mezzanine for daily
exercise. àthis is being done
- Buy a muscle stimulatoràdone.
- Perform aerobic exercises 2 days / week and strengthening exercises 2 days /
week. à when house is complete
- When
caffeine has been eliminated from my diet and some muscle tone improvement
seen, see a chiropractor. à within 6
weeks after starting exercises
Adjustments tend to become unadjusted when muscles are out of tone or too
tense. Within a few chiropractor visits I should be able to maintain alignment.
The neck and back exercises will need to be integrated into a complete exercise routine.
I need to further investigate the use of tens and microlight 830 for the neck and shoulder.
ADDITIONAL INFORMATION ON THE BACK
The following site – misdiagnosed Parkinson’s - is a one man tirade about doctors not understanding Parkinson’s. My opinion is that the doctors misdiagnosed the patients. The symptoms partially favor Parkinson’s symptoms but do not totally match. All the symptoms he describes are from a misaligned spine. His book would be excellent research if you have the symptoms he describes.
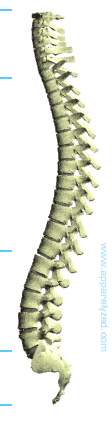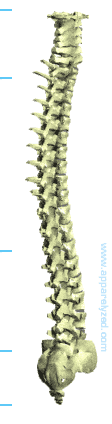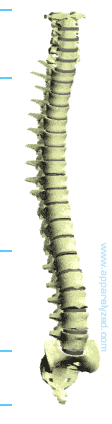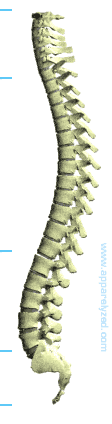
The Vertebral Column and Vertebrae
|
7cervical vertebrae
12 thoracic vertebrae
5 lumbar vertebrae
5 sacral & cocygeal (fused) |
|
The Vertebral Column (Spinal Column) supports the head and encloses the spinal cord.
The spinal column is comprised of 26 individual bones, these bones are refered to as vertebrae. The spinal column is divided into 5 different areas containing groups of vertebrae and are grouped as follows:
7 cervical vertebrae in the neck.
12 thoracic vertebrae in the upper back corresponding to each pair of ribs.
5 lumbar vertebrae in the lower back.
5 sacral vertebrae which are fused together to form 1 bone called the sacrum.
4 coccygeal vertebrae that are fused together to form the coccyx or tailbone.
The vertebrae are refered to by their name and number, counting down from the top of the spinal column as follows:
The cervical vertebrae are C1 - C7
The thoracic vertebrae are T1 –T12
The lumbar are L1 – L5
The sacrum and coccyx do not have numbers and each is thought of as one bone. Spinal nerves exit the sacrum and coccyx at levels (Foramen) within the main structure of each vertebra.
ELECTRICAL STIMULATION GUIDE AND DISCUSSION
NOTE: There is a difference in Transcutaneous Electrical Nerve Stimulation (TENS) and Electrical Muscle Stimulation (EMS). Tens is a lighter NERVE stimulation at higher frequencies with little or no movement and EMS is a stronger lower frequency signal for muscle contraction. Care must be taken, especially with very inflamed or weak muscles not to over stimulate. More harm than good can be done. The two test summaries below indicate that TENS/Exercise equally benefit the lower back and are better than massage.
Interferential stimulation (IFS) is a type of electrical stimulation that uses paired electrodes of two independent circuits carrying high-frequency (4000 Hz) and medium-frequency alternating currents. The superficial electrodes are aligned on the skin around the affected area. It is believed that IFS permeates the tissues more effectively and, with less unwanted stimulation of cutaneous nerves, is more comfortable than transcutaneous electrical stimulation (TENS). Interferential stimulation has been investigated as a technique to reduce pain, improve range of motion, or promote local healing following various tissue injuries. There are no standardized protocols for the use of interferential therapy; the therapy may vary according to the frequency of stimulation, the pulse duration, treatment time, and electrode-placement technique.
Transcutaneous Electrical Nerve Stimulation for Low Back Pain: (TENS) A Comparison of ( electrical pads) and Massage for Pain and Range of Motion
Dr. Melzack is Research Director of the Pain
Center, Montreal General Hospital, and Professor of Psychology, Department of
Psychology, McGill University, 1205 Docteur Penfield Ave, Montreal, Quebec,
Canada H3A 1B1.
Ms. Vetere was on leave as Research Associate, Physical Medicine Department,
Montreal General Hospital, when this article was written, and is now Staff
Physiotherapist, Montreal Convalescent Hospital, 6363 Hudson Rd, Montreal,
Quebec, Canada H3S 1M9.
Ms. Finch is Assistant Charge Therapist and Research Coordinator, Physical
Medicine Department, Montreal General Hospital, 1650 Cedar Ave, Montreal, Quebec,
Canada H3G 1A4.
Patients with acute or chronic low back pain were treated in a double-blind study that compared transcutaneous electrical nerve stimulation at intense levels and gentle, mechanically administered massage. Transcutaneous electrical nerve stimulation produced significantly greater pain relief, based on two measures of the McGill Pain Questionnaire, and significant improvement in straight leg raising. There were no significant differences between the two groups in back-flexion scores. Pain-relief scores and range-of-motion scores were significantly correlated. The results indicate that pain-relief scores provide valuable information and can easily be obtained from patients for whom pain is a major symptom.
A controlled trial of transcutaneous electrical nerve stimulation (TENS) and exercise for chronic low back pain
RA Deyo, NE Walsh, DC Martin, LS Schoenfeld, and S Ramamurthy
Abstract
A number of treatments are widely prescribed for chronic back pain, but few have been rigorously evaluated. We examined the effectiveness of transcutaneous electrical nerve stimulation (TENS), a program of stretching exercises, or a combination of both for low back pain. Patients with chronic low back pain (median duration, 4.1 years) were randomly assigned to receive daily treatment with TENS (n = 36), sham TENS (n = 36), TENS plus a program of exercises (n = 37), or sham TENS plus exercises (n = 36). After one month no clinically or statistically significant treatment effect of TENS was found on any of 11 indicators of outcome measuring pain, function, and back flexion; there was no interactive effect of TENS with exercise. Overall improvement in pain indicators was 47 percent with TENS and 42 percent with sham TENS (P not significant). The 95 percent confidence intervals for group differences excluded a major clinical benefit of TENS for most outcomes. By contrast, after one month patients in the exercise groups had significant improvement in self-rated pain scores, reduction in the frequency of pain, and greater levels of activity as compared with patients in the groups that did not exercise. The mean reported improvement in pain scores was 52 percent in the exercise groups and 37 percent in the nonexercise groups (P = 0.02). Two months after the active intervention, however, most patients had discontinued the exercises, and the initial improvements were gone. We conclude that for patients with chronic low back pain, treatment with TENS is no more effective than treatment with a placebo, and TENS adds no apparent benefit to that of exercise alone.
A transcutaneous electrical nerve stimulation (TENS) unit consists of 1 or more electrical-signal generators, a battery, and a set of electrodes. The TENS unit is small and programmable, and the generators can deliver trains of stimuli with variable current strengths, pulse rates, and pulse widths. The preferred waveform is biphasic, to avoid the electrolytic and iontophoretic effects of a unidirectional current. The usual settings for the stimulus parameters used clinically are the following:
- Amplitude - Current at a comfortable, low intensity level, just above threshold
- Pulse width (duration) - 10-1000 microseconds
- Pulse rate (frequency) - 80-100 impulses per second (Hz); 0.5-10 Hz when the stimulus intensity is set high
When TENS is used analgesically, patients are instructed to try different frequencies and intensities to find those that provide them with the best pain control. Optimal settings of stimulus parameters are subjective and are determined by trial and error. Electrode positioning is quite important. Usually, the electrodes are initially placed on the skin over the painful area, but other locations (eg, over cutaneous nerves, trigger points, acupuncture sites) may give comparable or even better pain relief.
The 3 options for the standard settings used in different therapeutic methods of TENS application include the following:
- Conventional TENS has a high stimulation frequency (40-150 Hz) and low intensity, just above threshold, with the current set between 10-30 mA. The pulse duration is short (up to 50 microseconds). The onset of analgesia with this setup is virtually immediate. Pain relief lasts while the stimulus is turned on, but it usually abates when the stimulation stops. Patients customarily apply the electrodes and leave them in place all day, turning the stimulus on for approximately 30-minute intervals throughout the day. In individuals who respond well, analgesia persists for a variable time after the stimulation stops.
- In acupuncturelike settings, the TENS unit delivers low frequency stimulus trains at 1-10 Hz, at a high stimulus intensity, close to the tolerance limit of the patient. Although this method sometimes may be more effective than conventional TENS, it is uncomfortable, and not many patients can tolerate it. This method often is considered for patients who do not respond to conventional TENS.
- Pulsed (burst) TENS uses low-intensity stimuli firing in high-frequency bursts. The recurrent bursts discharge at 1-2 Hz, and the frequency of impulses within each burst is at 100 Hz. No particular advantage has been established for the pulsed method over the conventional TENS method.
Patient comfort is a very important determinant of compliance and, consequently, of the overall success of treatment. The intensity of the impulse is a function of pulse duration and amplitude. Greater pulse widths tend to be more painful. The acupuncturelike method is less tolerable, because the impulse intensity is higher.
The amount of output current depends on
the combined impedance of the electrodes, skin, and tissues. With repetitive
electrical stimuli applied to the same location on the skin, the skin impedance
is reduced, which could result in greater current flow as stimulation
continues. A constant current stimulator, therefore, is preferred in order to
minimize sudden, uncontrolled fluctuations of current intensity related to
changes in impedance. An electroconductive gel applied between the electrode
and skin serves to minimize the skin impedance.
Medical complications arising from use of TENS are rare. However, skin
irritation can occur in as many as 33% of patients, due, at least in
part, to drying out of the electrode gel. Patients need to be instructed
in the use and care of TENS equipment, with particular attention to the
electrodes.
In some cases, individuals react to the tape used to secure the electrodes. Skin irritation is minimized by using disposable, self-adhesive electrodes and repositioning them slightly for repeated applications. The use of TENS is contraindicated in patients with a demand-type pacemaker, because the stimulus output of the TENS unit may drive or inhibit the pacemaker.
A variety of newer transcutaneous or percutaneous electrical stimulation modalities have emerged. They include the following:
- Interferential current therapy (IFC) is based on summation of 2 alternating current signals of slightly different frequency. The resultant current consists of a cyclical modulation of amplitude, based on the difference in frequency between the 2 signals. When the signals are in phase, they summate to an amplitude sufficient to stimulate, but no stimulation occurs when they are out of phase. The beat frequency of IFC is equal to the difference in the frequencies of the 2 signals. For example, the beat frequency and, hence, the stimulation rate of a dual channel IFC unit with signals set at 4200 and 4100 Hz is 100 Hz.
- IFC therapy can deliver higher currents than TENS can. IFC can use 2, 4, or 6 applicators, arranged in either the same plane, for use on such regions as the back, or in different planes in complex regions (eg, the shoulder).
- Percutaneous electrical nerve stimulation (PENS) combines advantages of electroacupuncture and TENS. Rather than using surface electrodes, PENS uses acupuncturelike needle probes as electrodes, with these placed at dermatomal levels corresponding to local pathology. The main advantage of PENS over TENS is that it bypasses local skin resistance and delivers electrical stimuli at the precisely desired level in close proximity to the nerve endings located in soft tissue, muscle, or periosteum.3
Applications of Tens in Clinical Practice
Literature on the effectiveness of transcutaneous electrical nerve stimulation (TENS) in a variety of medical conditions reports a wide range of outcomes, from very positive to negative. Currently, there is an overall consensus favoring the use of TENS, with authorities differing on its value in different clinical situations. Generally, TENS provides initial relief of pain in 70-80% of patients, but the success rate decreases after a few months or longer to around 20-30%. To exclude a false-negative response, a trial of TENS for at least 1 hour should be given to confirm potential benefit from subsequent continuous use.
According to Johnson, the time from the start of stimulation to the onset of analgesia varies from almost immediate to hours (on average, 20-30 minutes in over 75% of patients and 1 hour in 95% of patients).8 The duration of analgesia also varies considerably, continuing only for the duration of stimulation in some patients and providing considerable, prolonged poststimulation relief in others. The same TENS protocol may have different degrees of antinociception in acute experimental pain compared with chronic clinical pain in patients with chronic low back pain (LBP).9
Patients differ in their stimulus preferences and in their rates of compliance. In Johnson's study of compliance in patients who benefited from TENS, 75% used the device on a daily basis. Patients showed individual preferences for particular pulse frequencies and patterns, and they consistently adjusted their stimulators to these settings in subsequent treatment sessions.
Indications for the use of TENS
- Neurogenic pain (eg, deafferentation pain, phantom pain), sympathetically mediated pain, postherpetic neuralgia, trigeminal neuralgia, atypical facial pain, brachial plexus avulsion, pain after spinal cord injury (SCI)
- Musculoskeletal pain - Examples of specific diagnoses include joint pain from rheumatoid arthritis and osteoarthritis, acute postoperative pain (eg, postthoracotomy), and acute posttraumatic pain.10,11,12,13,14,15,16 After surgery, TENS is most effective for mild to moderate levels of pain, and it is ineffective for severe pain. The use of TENS in chronic LBP and myofascial pain is controversial, with placebo-controlled studies failing to show statistically significant beneficial results. Uncertainty also exists about the value of TENS in tension headache.
- Visceral pain and dysmenorrhea - TENS has been successfully applied to these conditions as well.17
- Other disorders - TENS has been used successfully in patients with angina pectoris and urge incontinence, as well as in patients requiring dental anesthesia.18,19 Reports discuss the use of TENS to assist patients in regaining motor function following stroke, to control nausea in patients undergoing chemotherapy, as an opioid -sparing modality in postoperative recovery, and in postfracture pain.20,21,22,23,24,25,26
Contraindications for the use of TENS
- TENS should not be used in patients with a pacemaker (especially of the demand type).
- TENS should not be used during pregnancy, because it may induce premature labor.
- TENS should not be applied over the carotid sinuses due to the risk of acute hypotension through a vasovagal reflex.
- TENS should not be placed over the anterior neck, because laryngospasm due to laryngeal muscle contraction may occur.
- The electrodes should not be placed in an area of sensory impairment (eg, in cases of nerve lesions, neuropathies), where the possibility of burns exists.
- A TENS unit should be used cautiously in patients with a spinal cord stimulator or an intrathecal pump.
TENS electrodes should never be placed:
- On or near the eyes
- In the mouth
- Transcerebrally (on each temple)
- On the front of the neck (due to the risk of acute hypotension through a vasovagal reflex)
- Directly on the groin such as on penis or testicles
- On areas of numb skin/decreased sensation
- On broken skin areas or wounds
- On or near the trigeminal nerve if you have a history of herpes zoster induced trigeminal neuralgia (Postherpetic neuralgia)
TENS should also be used with caution in people with epilepsy or pregnant women (do not use over area of the uterus as the effects of electrical stimulation over the developing fetus are not known). TENS should not be used by people with an artificial cardiac pacemaker due to risk of interference and failure of their implanted device. Possible failure of these warnings can result in a cardiac arrhythmia.
A number of studies have compared transcutaneous electrical nerve stimulation (TENS) with similar therapeutic modalities, including percutaneous electrical nerve stimulation (PENS), interferential current therapy (IFC), and acupuncture.17,27 The results included the following:
- In one study of elderly patients with chronic low back pain (LBP), acupuncture and TENS had demonstrable benefits, with the acupuncture group demonstrating improvement in spinal flexion.
- In patients with chronic LBP and sciatica, PENS was more effective than TENS in providing short-term pain relief and improved function, including an improved quality of sleep and sense of well-being.
- Overall, 91% and 73% of patients, respectively, chose PENS as the preferred modality for pain relief in LBP and sciatica.
- PENS has been used successfully for pain relief in patients with acute herpes zoster and in persons suffering from cancer with bony metastases.
- IFC and TENS had a statistically significant effect on the median nerve excitation threshold in young women.
Keywords
transcutaneous electrical nerve stimulation, TENS, TENS unit, transcutaneous, analgesia, electrical nerve stimulation, electrical stimulation, electrical stimulator, TENS units, TENS stimulator, TENS machine, low back pain, lower back pain, interferential, transcutaneous nerve stimulation, nerve stimulator, e stim, e-stim, TENS unit electrodes, TENS electrode, interferential stimulator, interferential stimulation, interferential therapy, interferential unit, percutaneous electrical nerve stimulation, PENS
Percutaneous Electrical Nerve Stimulation (PENS) for Low Back Pain (needles with electrical stimulation at an alternating frequency of 15 and 30 Hz)
A Randomized Crossover Study
El-sayed A. Ghoname, MD; William F. Craig, MD; Paul F. White, PhD, MD; Hesham E. Ahmed, MD; Mohamed A. Hamza, MD; Brent N. Henderson, PhD; Noor M. Gajraj, MD; Philip J. Huber, MD; Robert J. Gatchel, PhD
JAMA. 1999;281:818-823.
Context Low back pain (LBP) contributes to considerable disability and lost wages in the United States. Commonly used opioid and nonopioid analgesic drugs produce adverse effects and are of limited long-term benefit in the management of this patient population.
Objective To compare the effectiveness of a novel nonpharmacologic pain therapy, percutaneous electrical nerve stimulation (PENS), with transcutaneous electrical nerve stimulation (TENS) and flexion-extension exercise therapies in patients with long-term LBP.
Design A randomized, single-blinded, sham-controlled, crossover study from March 1997 to December 1997.
Setting An ambulatory pain management center at a university medical center.
Patients Twenty-nine men and 31 women with LBP secondary to degenerative disk disease.
Interventions Four therapeutic modalities (sham-PENS, PENS, TENS, and exercise therapies) were each administered for a period of 30 minutes 3 times a week for 3 weeks.
Main Outcome Measures Pretreatment and post treatment visual analog scale (VAS) scores for pain, physical activity, and quality of sleep; daily analgesic medication usage; a global patient assessment questionnaire; and Health Status Survey Short Form (SF-36).
Results PENS was significantly more effective in decreasing VAS pain scores after each treatment than sham-PENS, TENS, and exercise therapies (after-treatment mean ± SD VAS for pain, 3.4 ± 1.4 cm, 5.5 ± 1.9 cm, 5.6 ± 1.9 cm, and 6.4 ± 1.9 cm, respectively). The average ± SD daily oral intake of nonopioid analgesics (2.6±1.4 pills per day) was decreased to 1.3±1.0 pills per day with PENS (P<.008) compared with 2.5±1.1, 2.2±1.0, and 2.6±1.2 pills per day with sham-PENS, TENS, and exercise, respectively. Compared with the other 3 modalities, 91% of the patients reported that PENS was the most effective in decreasing their LBP. The PENS therapy was also significantly more effective in improving physical activity, quality of sleep, and sense of well-being (P<.05 for each). The SF-36 survey confirmed that PENS improved post treatment function more than sham-PENS, TENS, and exercise.
Conclusions In this sham-controlled study, PENS was more effective than TENS or exercise therapy in providing short-term pain relief and improved physical function in patients with long-term LBP.
Author Affiliations: Eugene McDermott Center for
Pain Management, Departments of Anesthesiology and Pain Management (Drs
Ghoname, Craig, White, Ahmed, Hamza, and Gajraj), Surgery (Dr Huber), and
Psychiatry (Drs Henderson and Gatchel), University of Texas Southwestern
Medical Center, Dallas.
Efficacy of Percutaneous Electrical Nerve Stimulation for the Treatment of Chronic Low Back Pain in Older Adults
Debra K. Weiner, MD,* † ‡ Thomas E. Rudy, PhD, † ‡ § Ronald M. Glick, MD, # J. Robert Boston, PhD, ‖ Susan J. Lieber, MS,OTR/L, ‡ Lisa A. Morrow, PhD, † and Stephen Taylor, DO ¶
*Department of Medicine, Division of Geriatric Medicine, † Department of Psychiatry, ‡ Department of Anesthesiology, § Department of Biostatistics, ‖ Department of Electrical Engineering, and # Department of Family Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania; and ¶ Department of Manipulative Medicine, University of North Texas Health Science Center at Fort Worth, Fort Worth, Texas.
Address correspondence to to Debra K. Weiner, MD, 5750 Center Avenue; Suite 400, Pittsburgh, PA 15206. E-mail: dweiner@pitt.edu
KEYWORDS
low back pain • aged • PENS • treatment outcomes
ABSTRACT
OBJECTIVES:To determine the efficacy of a complementary analgesic modality, percutaneous electrical nerve stimulation (PENS), for the treatment of chronic low back pain (CLBP) in community-dwelling older adults.
DESIGN:Randomized, controlled clinical trial.
SETTING:University of Pittsburgh Pain Evaluation and Treatment Institute.
PARTICIPANTS:Thirty-four English speaking, community-dwelling adults aged 65 and older with CLBP of at least moderate intensity experienced every day or almost every day.
INTERVENTION:Subjects were randomized to receive twice-weekly PENS and physical therapy (PT) or sham PENS and physical therapy for 6 weeks.
MEASUREMENTS:At baseline, immediately after the 6-week intervention period, and 3 months later, the primary outcome measures pain intensity and pain-related disability were assessed. The secondary outcome measures physical performance (timed chair rise, functional reach, gait speed, static and isoinertial lifting), psychosocial factors (mood, sleep, and life control), and cognitive function (measures of attention, concentration, and mental flexibility) were also collected.
RESULTS:Subjects randomized to PENS plus PT displayed significant reductions in pain intensity measures from pre- to post treatment (P < .001), but the sham PENS plus PT group did not (P = .94). These pain reduction effects were maintained at 3-month follow-up. Similarly, significant reductions in pain-related disability were observed at post treatment (P = .002) for the PENS plus PT group and were maintained at follow-up, but the sham PENS plus PT group did not show reductions in pain-related disability (P = .81). Of the secondary outcome measures, psychosocial function, timed chair rise, and isoinertial lifting endurance also improved significantly at post treatment for the PENS plus PT group, and their improvement was sustained at 3-month follow-up, but the sham PENS plus PT did not display significant changes on these measures after treatment.
CONCLUSION:This preliminary study suggests that PENS may be a promising treatment modality for community-dwelling older adults with CLBP, as demonstrated by reduction in pain intensity and self-reported disability, and improvement in mood, life control, and physical performance. Larger studies with longer duration of follow-up are needed to validate these findings and support the use of PENS in clinical practice.
NOTE: PENS is more effective than TENS. The difference is that PENS is applied at the acupuncture points.
Low Level Laser Stimulation – (LLLS)
Cold Laser Therapy (e.g. ML 830® Laser) 5-6 minutes 10 times together with manual therapy.
In the late 1960's, researchers introduced the concept of laser biostimulation using low-powered laser beams to produce non-thermal effects in human tissue. The first experimental applications of low-level energy laser therapy were reported in 1968, when researchers used ruby and argon lasers on non-healing or slow-to-heal ulcers. Later research substantiated the efficacy of laser treatment to accelerate the healing of wounds, attenuate pain, and reduce tissue inflammation in both humans and animals.
To treat chronic pain with laser biostimulation, one must reach deep into tissue to irradiate the affected area. Laser wavelengths between 820 nanometers to 840 nanometers have an extremely low absorption rate in human tissue, thus allowing deep penetration of laser light. The 830 nm laser beam is also well absorbed in subcellular organelles, causing them to function normally. The laser's low level of power output also affects the depth of the beam's penetration, and has been shown to be effective in treating human tissue. The 830 nm laser with a power output between 60 milliwatts (mW) and 90 mW is reported by experimenting clinicians to be optimal for treating chronic pain.
Featured Articles
ADVANCE
for Physical Therapists & PT Assistants
Noninvasive, Low Energy Laser
Treatment Calms Carpal Tunnel Syndrome
MICROLIGHT CORPORATION OF AMERICA
Michael M. Barbour, President
2935 Highland Lakes
Missouri City, Texas 77459
Phone: 281-433-4648
Customer Service: 713-520-0668
email: mbarbour@microlightcorp.com
$3000 or $35-$45 and takes 10-15 treatments.
FDA approved
Steve Barbour 713-927-7068
The Color Atlas of Acupuncture
Acupuncture Points and Meridians
Anatomy Trains and Meridians This book pulls all sciences together.
What can cause low back injuries?
What can I do for relief when I've hurt my lower back?
What else can I do for relief?
Is there relief for ongoing back problems?
What's the best position for standing?
What's the best position for sleeping?
What exercises can I do to strengthen my back?
CHIROPRACTOR S
NUCCA CERTIFIED
Houston Spinal Care Toll-Free at 1-888-446-6896
Dr. Robert Ramirez
Certification
Candidate - Passed Level I
5715 Northwest Central Dr.
Ste F-111
Houston, TX 77092
Phone: 713-690-4150
Fax: 713-690-4175
Email: DrRob@hspinalcare.com
Years In Practice: 7
http://www.hspinalcare.com
Low Back Pain Exercise Guide
Regular exercises to restore the strength of your back and a gradual return to everyday activities are important for your full recovery. Your orthopaedic surgeon and physical therapist may recommend that you exercise 10 to 30 minutes a day 1 to 3 times a day during your early recovery. They may suggest some of the following exercises. This guide can help you better understand your exercise and activity program, which should be supervised by your therapist and orthopaedic surgeon.
Ankle Pumps
1. Lie on your back.
2. Move ankles up and down. Repeat 10 times.
3. Repeat 10 times.
Heel Slides
1. Lie on your back.
2. Slowly bend and straighten knee.
3. Repeat 10 times.
Abdominal Contraction
1. Lie on your back with knees bent and hands resting below ribs.
2. Tighten abdominal muscles to squeeze ribs down toward back.
3. Be sure not to hold breath.
4. Hold 5 seconds.
5. Relax.
6. Repeat 10 times.
Wall Squats
1. Stand with back leaning against wall.
2. Walk feet 12 inches in front of body.
3. Keep abdominal muscles tight while slowly bending both knees 45 degrees.
4. Hold 5 seconds.
5. Slowly return to upright position.
6. Repeat 10 times.
Heel Raises
1. Stand with weight even on both feet.
2. Slowly raise heels up and down.
3. Repeat 10 times.
Straight Leg Raises
1. Lie on your back with one leg straight and one knee bent.
2. Tighten abdominal muscles to stabilize low back.
3. Slowly lift leg straight up about 6 to 12 inches and hold 1 to 5 seconds.
4. Lower leg slowly.
5. Repeat 10 times.
Single Knee to Chest Stretch
1. Lie on your back with both knees bent.
2. Hold thigh behind knee and bring one knee up to chest.
3. Hold 20 seconds.
4. Relax.
5. Repeat 5 times on each side.
Hamstring Stretch
1. Lie on your back with legs bent.
2. Hold one thigh behind knee.
3. Slowly straighten knee until a stretch is felt in back of thigh.
4. Hold 20 seconds.
5. Relax.
6. Repeat 5 times on each side.
Lumbar Stabilization Exercises With Swiss Ball
Abdominal muscles must remain contracted during each exercise (see Abdominal Contraction). Perform each exercise for 60 seconds. The farther the ball is from your body, the harder the exercise.
Lying on Floor
1. Lie on your back with knees bent and calves resting on ball.
2. Slowly raise arm over head and lower arm, alternating right and left sides.
3. Slowly straighten one knee and relax, alternating right and left sides.
4. Slowly straighten one knee and raise opposite arm over head. Alternate opposite arms and legs.
5. Slowly "walk" ball forward and backward with legs.
Sitting on Ball
1. Sit on ball with hips and knees bent 90°and feet resting on floor.
2. Slowly raise arm over head and lower arm, alternating right and left sides.
3. Slowly raise and lower heel, alternating right and left sides.
4. Slowly raise one heel and raise opposite arm over head. Alternate opposite arm and heel.
5. Marching: Slowly raise one foot 2 inches from floor, alternating right and left sides.
Standing
1. Stand with ball between your low back and wall.
2. Slowly bend knees 45 ° to 90 ° . Hold 5 seconds. Straighten knees.
3. Slowly bend knees 45 ° to 90 ° while raising both arms over head.
Lying on Ball
1. Lie on your stomach over ball
2. Slowly raise alternate arms over head.
3. Slowly raise alternate legs 2 to 4 inches from floor.
4. Combine 1 and 2, alternating opposite arms and legs.
5. Bend one knee. Slowly lift this leg up, alternating right and left legs.
NOTE: Be careful not to arch your low back!
Advanced Exercise Program
Hip Flexor Stretch
1. Lie on your back near edge of bed, holding knees to chest.
2. Slowly lower one leg down, keeping knee bent, until a stretch is felt across top of the hip/thigh.
3. Hold 20 seconds.
4. Relax.
5. Repeat 5 times on each side.
Piriformis Stretch
1. Lie on back with both knees bent.
2. Cross one leg on top of the other.
3. Pull opposite knee to chest until a stretch is felt in the buttock/hip area.
4. Hold 20 seconds.
5. Relax.
6. Repeat 5 times each side.
Lumbar Stabilization Exercise With Swiss Ball
1. Lie on stomach over ball.
2. " Walk " hands out in front of ball until ball is under legs. Reverse to starting position.
3. " Walk " hands out in front of ball until ball is under legs and slowly raise alternating arms over head.
4. " Walk " hands out in front of ball and slowly perform push-ups.
Maintain spine in neutral position while stabilizing with abdominal muscles to protect the low back during aerobic exercise.
- Stationary bike for 20 to 30 minutes.
- Treadmill for 20 to 30 minutes.
BACK PAIN.HTM